Introduction
In recent years, the field of organ transplantation has made tremendous strides to pioneering organ care technology and bio-printing innovations. These advancements have revolutionized the way organs are preserved, transported, and implanted, leading to healthier futures for countless individuals awaiting life-saving transplants.
Organ care technology, often referred to as "ex-vivo" or "organ perfusion" technology, has transformed the traditional method of organ preservation. In the past, organs were harvested from a deceased donor and transported in an ice-cold solution to the recipient. This method often led to organ damage and limited the time an organ could be stored before transplantation. However, with the introduction of organ care technology, organs can now be kept in a near-physiological state outside of the body. This technology allows the organs to receive oxygen, nutrients, and medications, mimicking the conditions of the human body. As a result, the organs can be preserved for longer periods, increasing the chances of a successful transplant and reducing the risk of rejection.
Another groundbreaking innovation in the field of organ transplantation is bio-printing. Bio-printing involves creating three-dimensional structures using living cells, which can be used to generate functional organs. This revolutionary technology can potentially eliminate the shortage of donor organs, as organs can be created in the lab using a patient's cells. With bio-printing, transplants become more readily available, and the risk of rejection is significantly reduced.
The impact of these advancements in organ care technology and bio-printing innovations cannot be overstated. Patients facing life-threatening conditions can now have hope for a healthier future, as they no longer have to rely solely on the limited availability of donor organs. These technologies have the potential to transform the field of transplantation and revolutionize personalized medicine. As further research and development continues, the possibilities for healthier futures are endless.
Data Bridge Market Research analyses that the organ transplantation market is expected to grow at a CAGR of 9.36% during the forecast period. The "kidney" accounts for the largest application segment in the organ transplantation market within the forecasted period.
To know more, visit https://www.databridgemarketresearch.com/reports/global-organ-transplantation-market
The Challenge of Organ Transplantation/ Limitations and Risks of Traditional Organ Transplants-
- Organ shortage: One of the most significant challenges in organ transplantation is the severe shortage of organs available for transplantation compared to the growing demand. The number of individuals awaiting organ transplants far exceeds the number of available organs, resulting in long waiting lists and a high mortality rate among patients.
- Organ rejection: The human immune system naturally tends to recognize and reject foreign tissues or organs. Despite advancements in immunosuppressive drugs, organ rejection remains a major hurdle in successful transplantation. Patients often require lifelong immunosuppressive therapy, which can have various side effects and increase the risk of infections and other complications.
- Organ preservation: Organs are extremely delicate and susceptible to damage and deterioration during transplantation. The limited timeframe for organ preservation before transplantation poses a significant challenge, as organs need to be transported quickly and maintained in optimal conditions to ensure their viability.
- Surgical complications: The surgical procedure itself poses risks and challenges. Organ transplantation surgeries are complex and intricate, requiring high surgical expertise and precision. Complications such as bleeding, infection, and organ damage can occur during the surgical process, potentially compromising the success of the transplantation.
- Ethical and legal Issues: Organ transplantation raises ethical and legal dilemmas concerning organ procurement and allocation. Fair and equitable distribution of organs is a complex task, and policies and regulations vary across countries and regions. Ethical concerns regarding living organ donation, consent, and the commercialization of organs further complicate the transplantation landscape.
- Long-term organ function: While transplantation can offer a new lease on life for patients, long-term organ function remains a challenge. Transplanted organs may experience complications, such as organ dysfunction, rejection, or the development of other diseases over time. Continuous monitoring and follow-up care are essential to ensure the long-term success and survival of transplanted organs.
The Growing Demand for Organs-
Aging population: As the global population ages, there is a higher prevalence of age-related diseases that can lead to organ failure, such as kidney disease, liver disease, and heart disease. This demographic shift increases the number of individuals in need of organ transplants.
Chronic diseases: The rise in chronic diseases, including diabetes, hypertension, and respiratory conditions, has contributed to an increased demand for organ transplants. These conditions can progress to end-stage organ failure, necessitating transplantation as a treatment option.
Improved transplant outcomes: Advances in medical technology, surgical techniques, and post-transplant care have significantly improved the success rates of organ transplants. This has led to increased confidence in transplantation as a viable treatment option, resulting in more individuals seeking organ transplants.
Awareness and education: Increased awareness and education about organ donation and transplantation have positively influenced public perception and acceptance of organ transplantation. Efforts to promote organ donation and dispel myths surrounding transplantation have led to more individuals expressing their willingness to donate organs and avail themselves of transplantation if needed.
Introduction to Organ Care Technology as a Solution
Organ Care Technology (OCT) emerges as a groundbreaking solution in organ transplantation, revolutionizing how organs are preserved, transported, and transplanted. It represents a significant leap forward in addressing the challenges associated with traditional organ transplantation. OCT encompasses a range of innovative techniques and devices designed to optimize organ viability, enhance transplant outcomes, and ultimately save more lives.
At its core, OCT focuses on providing organs with an environment that closely mimics the conditions inside the human body, thereby extending their functional lifespan outside the donor. Utilizing specialized machines and solutions, organs can be perfused and preserved with oxygen, nutrients, and other essential factors controlled and monitored. This process maintains the organ's viability and allows for assessment and optimization of its condition before transplantation.
One of the key advantages of OCT is its ability to significantly extend the preservation time of organs compared to traditional cold storage methods. This expanded window provides more flexibility in organ transportation, enables coordination with recipient surgical teams, and reduces the risk of organ damage or complications. Additionally, OCT allows for the utilization of organs that were previously deemed unsuitable for transplantation due to limitations in cold storage preservation.
Furthermore, OCT enables the assessment and optimization of organ function in real-time. Medical professionals can identify any issues or signs of organ rejection early on by monitoring various parameters, such as oxygen levels, temperature, and pressure. This early detection allows for timely interventions, adjustments, or even the selection of alternative organs, improving the overall success rates of transplantation.
Organ Care Technology holds immense promise in addressing the critical shortage of organs, reducing waiting times for patients, and improving transplant outcomes. As this transformative approach continues to evolve and gain traction, it offers hope for a future where organ transplantation becomes more accessible, efficient, and successful, ultimately saving countless lives and transforming the landscape of healthcare.
Organ Care Technology: A Game-Changer
The Basics of Organ Perfusion and Preservation
Perfusion: Organ perfusion involves the continuous supply of oxygenated blood or specialized preservation solution to the organ to maintain its metabolic activity. Perfusion is typically achieved using a perfusion machine, which is designed to replicate the physiological conditions of the human body. The machine pumps the oxygenated blood or preservation solution through the organ's blood vessels, delivering nutrients and removing waste products.
Preservation solution: The preservation solution used in organ perfusion is a specially formulated solution that contains electrolytes, nutrients, and other additives to maintain the organ's cellular function. It helps prevent cellular damage, maintain pH balance, and minimize edema during preservation. The composition of the preservation solution may vary depending on the specific organ being preserved and the perfusion technique employed.
Organ preservation market is expected to gain market growth in the forecast period of 2022 to 2029. Data Bridge Market Research analyses the market to grow at a CAGR of 7.98%
To know more, visit https://www.databridgemarketresearch.com/reports/global-organ-preservation-market
Temperature control: Temperature control is a critical aspect of organ preservation. The organ is typically maintained at a specific temperature, often around physiological body temperature, to minimize cellular metabolism and reduce the risk of injury. Cooling methods, such as cold perfusion or hypothermic preservation, are commonly employed to slow down metabolic processes and extend the preservation time.
Monitoring and assessment: Various parameters are closely monitored during organ perfusion and preservation to ensure the organ's viability. These parameters may include oxygen levels, temperature, pH, perfusion pressure, and organ function. Continuous monitoring allows medical professionals to detect any deviations from normal parameters and take appropriate actions to optimize the organ's condition.
Healthcare automation streamlines processes and improves patient outcomes through technology.
Transport: Organ perfusion and preservation techniques also facilitate the transportation of organs from the donor to the recipient's surgical center. The optimized preservation conditions and extended preservation time provided by perfusion systems allow for greater flexibility in logistics, ensuring the organ reaches the recipient in an optimal condition for transplantation.
Advantages of Organ Care Systems
Extended preservation time: Organ care systems allow a significantly longer preservation time than traditional cold storage methods. This extended preservation window provides more flexibility in transportation logistics and enables better coordination with recipient surgical teams, reducing the risk of organ damage and complications.
Enhanced organ quality: Closely replicating the physiological conditions of the human body, organ care systems help maintain the organ's function and viability at a higher level. The continuous perfusion of oxygen, nutrients, and specialized preservation solutions ensures optimal conditions for the organ, minimizing ischemic injury and improving the overall quality of the organ.
Real-time monitoring and assessment: Organ care systems enable continuous monitoring and assessment of various parameters such as oxygen levels, temperature, pH, and organ function. This real-time monitoring allows for the early detection of any issues or signs of organ rejection. Medical professionals can make timely interventions, adjust the preservation conditions, or even choose alternative organs if necessary, improving transplant outcomes.
Individualized organ optimization: Organ care systems provide the opportunity for individualized organ optimization. The ability to monitor and adjust parameters specific to each organ allows for tailored preservation techniques. This customization ensures that each organ receives the ideal conditions for preservation, maximizing its chances of successful transplantation.
Expanded donor pool: Organ care systems can expand the pool of potential organ donors by making use of organs that may have been previously considered unsuitable for transplantation. For example, organs from donors with extended criteria, such as older donors or those with certain medical conditions, can be preserved and assessed more effectively, potentially increasing the number of available organs for transplantation.
Improved transplant outcomes: The combination of extended preservation time, enhanced organ quality, and real-time monitoring offered by organ care systems ultimately leads to improved transplant outcomes. Organs that have been preserved using these advanced techniques have a higher likelihood of successful transplantation, reduced risk of complications, and improved long-term function.
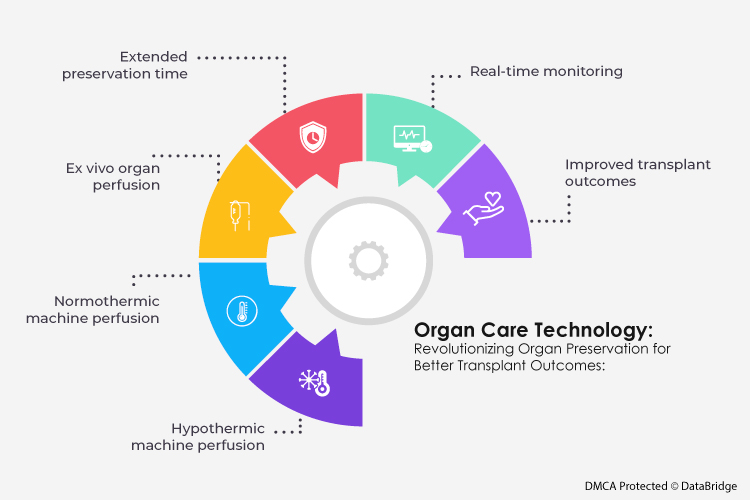
Organ Care Technology: Revolutionizing Organ Preservation for Better Transplant Outcomes
- Hypothermic machine perfusion: Improved organ preservation through controlled cooling
- Normothermic machine perfusion: Mimicking physiological conditions for optimal organ preservation
- Ex vivo organ perfusion: Transplantation of organs into a perfusion system for assessment
- Extended preservation time: Increased viability and flexibility for organ transportation
- Real-time monitoring: Continuous assessment of organ function and viability
- Improved transplant outcomes: Enhanced success rates and reduced complications
Notable Advances in Organ Care Technology
- Hypothermic Machine Perfusion: Hypothermic machine perfusion is an advanced organ care technology that involves the preservation of organs at lower temperatures (typically around 4°C) while supplying a controlled flow of oxygenated perfusion solution. This technique helps maintain the viability and functionality of organs, such as kidneys, livers, and hearts, during transportation and before transplantation. Providing oxygen and nutrients to the organ minimizes ischemic injury and allows for extended preservation time, improving the overall success rates of transplantation.
- Normothermic Machine Perfusion: Normothermic machine perfusion is a technique that involves maintaining organs at near-normal body temperature (typically around 37°C) and continuously perfusing them with a specialized solution. This approach allows for a more physiological environment compared to traditional cold storage methods, providing better organ preservation and assessment. Normothermic perfusion promotes cellular metabolism, reduces ischemic injury, and enables real-time monitoring of organ function, making it particularly useful for assessing organ viability, repairing damaged tissue, and optimizing organ quality prior to transplantation.
- Ex Vivo Organ Perfusion: Ex vivo organ perfusion refers to the transplantation of organs into a perfusion system outside of the human body for preservation and assessment. This technique allows for extended preservation time and offers a platform for assessing organ function, viability, and suitability for transplantation. Ex vivo perfusion systems provide a controlled environment where the organ can be monitored, treated, and optimized. This approach has the potential to increase the pool of viable organs for transplantation by allowing for evaluation and rehabilitation of marginal or previously deemed unsuitable organs, improving the overall success and outcomes of transplantation procedures.
Case Studies and Success Stories
Bio-Printing: Constructing the Future of Transplants
A. Introduction to Bio-Printing
Bio-printing, also known as 3D bioprinting, is an emerging technology that combines principles of 3D printing with biological materials to create functional living structures. It involves the precise layer-by-layer deposition of bioinks, which are composed of living cells, biomaterials, and growth factors, to build tissue-like structures. Bio-printing holds immense potential for regenerative medicine, enabling the fabrication of complex tissues and organs for transplantation, drug testing, and disease modeling. Bio-printing aims to address organ shortages, improve patient outcomes, and advance our understanding of human biology and disease by mimicking the natural architecture and cellular composition of tissues.
B. The Process of Bio-Printing
- Selection and Sourcing of Bio-Inks: The first step in bio-printing is carefully selecting and sourcing bio-inks. Bio-inks are formulated materials that contain living cells, biomaterials, and growth factors. The choice of bio-ink depends on the desired tissue or organ being printed. Researchers and scientists must consider factors such as cell type, compatibility with the printing system, mechanical properties, and ability to promote cell viability and tissue development. Bio-inks can be derived from the patient's own cells (autologous) or from cell cultures (allogeneic), and the sourcing process involves obtaining high-quality, well-characterized cells for incorporation into the bio-ink formulation.
- Designing the Organ Blueprint: The next step involves creating a digital blueprint or 3D model of the organ or tissue structure to be printed. Computer-aided design (CAD) software is used to design the organ's desired shape, architecture, and dimensions. This blueprint serves as a guide for the bio-printer, providing instructions on how the layers of bio-ink should be deposited to create the final structure. The design process considers factors such as vascularization, cell organization, and structural integrity to ensure the printed organ or tissue functions properly.
- Layer-by-Layer Printing: The actual bio-printing process involves layer-by-layer deposition of the bio-ink to create the desired structure. The bio-printer, equipped with specialized printing nozzles or extruders, follows the instructions from the organ blueprint to precisely deposit the bio-ink in a controlled manner. Depending on the bio-ink and printing system used, the printer may use various techniques, including extrusion-based, droplet-based, or laser-assisted methods. Each layer is carefully printed and positioned on top of the previous layer, gradually building the three-dimensional structure of the organ. This layer-by-layer approach ensures accuracy, structural integrity, and proper alignment of the printed cells and biomaterials.
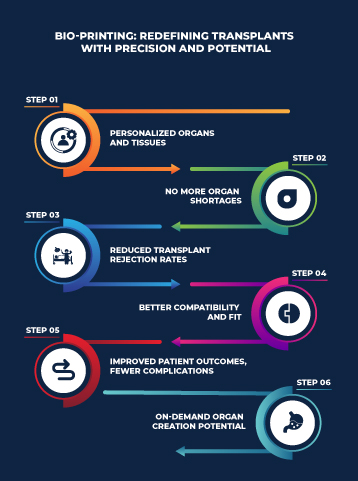
Bio-Printing: Redefining Transplants with Precision and Potential:
- Customization and personalization of organs and tissues
- Elimination of organ shortages and waiting lists
- Reduction of transplant rejection rates
- Enhanced compatibility and fit of transplanted organs
- Improved patient outcomes and reduced complications
- Potential for creating organs on-demand
C. Advantages and Potential of Bio-Printing
- Customization and Personalization: Bio-printing offers the potential to customize and personalize organs and tissues. Each patient may have unique anatomical features or specific requirements, and bio-printing allows for the creation of tailored organs that match the patient's individual needs. This customization improves the compatibility and fit of the transplanted organ, potentially enhancing patient outcomes and reducing the risk of complications.
- Eliminating Organ Shortages and Waiting Lists: Organ shortages and long waiting lists for transplants are major challenges in healthcare. Bio-printing has the potential to address this issue by providing an alternative source of organs. With the ability to create organs on-demand, bio-printing can significantly reduce the reliance on traditional organ donors. This has the potential to save countless lives and alleviate the burden on transplant waiting lists, improving access to life-saving treatments for patients in need.
- Reduction of Transplant Rejection: Transplant rejection is a significant concern in organ transplantation. Bio-printing offers the advantage of using a patient's own cells (autologous cells) for bio-ink, minimizing the risk of rejection. Using the patient's own cells, the immune response and the need for immunosuppressive drugs can be reduced, leading to better patient outcomes. Additionally, bio-printing techniques can incorporate biomaterials that promote tissue integration, further reducing the risk of rejection and improving the long-term success of organ transplants.
D. Challenges and Future Prospects
- Ensuring Structural Integrity and Functionality: One key challenge in bio-printing is ensuring that the printed organs possess the necessary structural integrity and functionality. The printed tissues and organs must be able to withstand physiological forces, maintain their shape, and perform their intended functions. Researchers and scientists focus on optimizing the bio-ink formulation, printing parameters, and post-printing processes to enhance cell viability, promote tissue maturation, and achieve the desired mechanical properties. This ensures that the bio-printed organs can effectively integrate and function within the recipient's body.
- Integration of Bio-Printed Organs into the Body: Successful integration of bio-printed organs into the recipient's body is crucial for long-term functionality. Factors such as vascularization, immune response, and cellular interactions need to be considered. Strategies such as pre-vascularization, in which blood vessels are incorporated into the bio-printed structure, and bioactive materials that promote cell adhesion and tissue integration are being explored. The goal is to ensure that the bio-printed organs establish proper connections with the recipient's existing tissues and organs, enabling functional integration and long-term viability.
- Regulatory and Ethical Considerations: The development and implementation of bio-printed organs raise important regulatory and ethical considerations. Regulatory bodies need to establish guidelines and standards to ensure the safety, efficacy, and quality of bio-printed organs for clinical use. Ethical considerations include issues such as informed consent, fair allocation of resources, and potential challenges related to intellectual property and affordability. Striking the right balance between innovation, patient safety, and ethical concerns is crucial for the responsible advancement and adoption of bio-printed organs in healthcare.
Collaborative Innovations and Research Efforts
- Partnerships between Industry and Academia: Collaboration between industry and academia plays a vital role in driving innovation and advancing research. Partnerships allow for the exchange of expertise, resources, and technologies. Industry brings real-world applications, commercialization capabilities, and funding, while academia contributes scientific knowledge, specialized facilities, and research capabilities. These collaborations foster the translation of academic research into practical solutions, accelerating the development of bio-printing technologies and applications
- Government Initiatives and Funding: Government initiatives and funding are crucial drivers for bio-printing advancements. Governments around the world support research and development in regenerative medicine and bio-printing through grants, subsidies, and funding programs. These initiatives promote scientific discovery, encourage collaboration between academia and industry, and provide financial resources for infrastructure development and clinical trials. Government support ensures a conducive environment for innovation, accelerates technology adoption, and helps overcome financial barriers to progress in the field
- Promising Research and Development Projects: Ongoing research and development projects in bio-printing contribute significantly to advancements in the field. Scientists and researchers explore novel materials, printing techniques, and bio-ink formulations. They investigate tissue-specific bio-printing approaches, optimize organ maturation processes, and develop new cellular manipulation and integration technologies. Promising projects drive innovation, generate scientific knowledge, and pave the way for the translation of bio-printing technologies into clinical applications.
- International Collaboration and Knowledge Sharing: International collaboration and knowledge sharing are crucial for advancing bio-printing globally. Scientists, researchers, and institutions from different countries exchange ideas, research findings, and best practices. Collaborative efforts enable the pooling of resources, expertise, and diverse perspectives. International conferences, symposiums, and research networks facilitate the dissemination of knowledge, promote collaboration, and foster standardization in bio-printing methodologies. Working together, the global bio-printing community can collectively address challenges, share advancements, and accelerate progress in the field
Ethical, Legal, and Social Implications
- Ethical Considerations of Organ Procurement and Bio-Printing: Organ procurement and bio-printing raise significant ethical considerations. Organ procurement involves issues such as informed consent, fairness in organ allocation, and avoiding exploitation of vulnerable populations. Bio-printing present's ethical challenges related to the sourcing and use of cells, potential human enhancement, and the blurring of natural and artificial boundaries. Ethical frameworks should ensure respect for autonomy, equity in access to transplantation, transparency in practices, and the prioritization of patient well-being
- Legal Frameworks and Regulations: Legal frameworks and regulations are essential for governing organ procurement and bio-printing. They provide guidance on consent, organ donation, intellectual property, safety, and quality standards. These frameworks ensure compliance with ethical principles, establish safeguards against unethical practices, and protect patient rights. Clear regulations promote responsible innovation, ensure patient safety, and maintain public trust in the integrity of organ procurement and bio-printing activities
- Addressing Social Disparities in Access to Transplants: Social disparities can create barriers to equitable access to organ transplants. Efforts should be made to address these disparities by increasing organ donation rates, improving organ allocation systems, and enhancing healthcare infrastructure in underserved areas. This involves initiatives to raise awareness about organ donation, educate communities about transplant eligibility, and advocate for fair and inclusive policies. Addressing social disparities, we can strive for equal access to life-saving treatments and work towards a more just and equitable healthcare system
Conclusion
The advancements in organ care technology (OCT) and bio-printing hold immense promise in addressing the challenges of organ transplantation. OCT focuses on optimizing organ viability, enhancing transplant outcomes, and expanding the pool of viable organs through machine perfusion and ex vivo organ preservation techniques. Bio-printing enables the creation of complex tissues and organs using bio-inks containing living cells. It offers customization, potential solutions to organ shortages, and reduced rejection rates. However, ongoing challenges include ensuring structural integrity, successful integration into the body, and navigating regulatory and ethical considerations. Addressing these issues and promoting responsible implementation, we can revolutionize the field of organ transplantation and improve patient outcomes. Collaboration between industry and academia, government initiatives, ongoing research projects, and international collaboration are essential for driving innovation in bio-printing and organ care technology. These partnerships facilitate the exchange of knowledge and resources, leading to the development of effective regulatory frameworks and responsible innovation practices. With these collaborative efforts, the field of organ transplantation can overcome challenges, improve patient outcomes, address organ shortages, and transform the landscape of healthcare.